Cataract
What is a cataract?
A cataract is a clouding of the lens in the eye that affects vision. Most cataracts are related to aging. Cataracts are very common in older people. By age 80, more than half of all Americans have either a cataract or have had cataract surgery. A cataract can occur in either or both eyes. It cannot spread from one eye to the other.
What is lens?
The lens is a clear part of the eye that helps to focus light, or an image, on the retina. The retina is the light-sensitive tissue at the back of the eye.
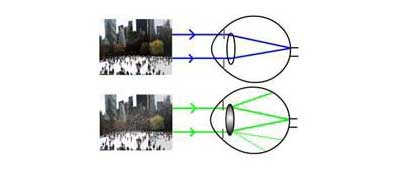
In a normal eye, light passes through the transparent lens to the retina. Once it reaches the retina, light is changed into nerve signals that are sent to the brain. The lens must be clear for the retina to receive a sharp image. If the lens is cloudy from a cataract, the image you see will be blurred
How do cataracts develop?
Age-related cataracts develop in two ways:
- Clumps of protein reduce the sharpness of the image reaching the retina. The lens consists mostly of water and protein. When the protein clumps up, it clouds the lens and reduces the light that reaches the retina. The clouding may become severe enough to cause blurred vision. Most age-related cataracts develop from protein clumpings. When a cataract is small, the cloudiness affects only a small part of the lens.You may not notice any changes in your vision. Cataracts tend to "grow" slowly, so vision gets worse gradually. Over time, the cloudy area in the lens may get larger, and the cataract may increase in size. Seeing may become more difficult.Your vision may get duller or blurrier.
- The clear lens slowly changes to a yellowish/brownish color, adding a brownish tint to vision. As the clear lens slowly colors with age, your vision gradually may acquire a brownish shade. At first, the amount of tinting may be small and may not cause a vision problem. Over time, increased tinting may make it more difficult to read and perform other routine activities. This gradual change in the amount of tinting does not affect the sharpness of the image transmitted to the retina. If you have advanced lens discoloration, you may not be able to identify blues and purples.
Who is at risk for cataract?
- The risk of cataract increases as you get older. Other risk factors for cataract include
- Certain diseases (for example, diabetes).
- Personal behavior (smoking, alcohol use).
- The environment (prolonged exposure to ultraviolet sunlight)
What are the symptoms of a cataract?
The most common symptoms of a cataract are:
- Cloudy or blurry vision.
- Colors seem faded.
- Glare. Headlights, lamps, or sunlight may appear too bright. A halo may appear around lights.
- Poor night vision
- Double vision or multiple images in one eye. (This symptom may clear as the cataract gets larger.)
- Frequent prescription changes in your eyeglasses or contact lenses
- These symptoms also can be a sign of other eye problems. If you have any of these symptoms, check with your eye care professional
Are there other types of cataract?
Yes. Although most cataracts are related to aging, there are other types of cataract:
Secondary cataract. Cataracts can form after surgery for other eye problems, such as glaucoma. Cataracts also can develop in people who have other health problems, such as diabetes. Cataracts are sometimes linked to steroid use.
Traumatic cataract. Cataracts can develop after an eye injury, sometimes years later.
Congenital cataract. Some babies are born with cataracts or develop them in childhood, often in both eyes. These cataracts may be so small that they do not affect vision. If they do, the lenses may need to be removed.
Radiation cataract. Cataracts can develop after exposure to some types of radiation.
How is a cataract detected?
Cataract is detected through a comprehensive eye exam that includes:
Visual acuity test. This eye chart test measures how well you see at various distances.
Dilated eye exam. Drops are placed in your eyes to widen, or dilate, the pupils.Your eye care professional uses a magnifying lens to examine your retina and optic nerve for signs of damage and other eye problems. After the exam, your close-up vision may remain blurred for several hours.
Tonometry. An instrument measures the pressure inside the eye. Numbing drops may be applied to your eye for this test.
Your eye care professional also may do other tests to learn more about the structure and health of your eye.
How is a cataract treated?
Removing the clouded lens and implanting an artificial lens is the only treatment for cataract, whcih is a simple procedure that takes just 20 minutes.
A cataract needs to be removed only when vision loss interferes with your everyday activities, such as driving, reading, or watching TV. You and your eye care professional can make this decision together. Once you understand the benefits and risks of surgery, you can make an informed decision about whether cataract surgery is right for you. In most cases, delaying cataract surgery will not cause long-term damage to your eye or make the surgery more difficult.You do not have to rush into surgery.
Sometimes a cataract should be removed even if it does not cause problems with your vision. For example, a cataract should be removed if it prevents examination or treatment of another eye problem, such as age-related macular degeneration or diabetic retinopathy.
If you have cataracts in both eyes that require surgery, the surgery will be performed on each eye at separate times, usually four to eight weeks apart.
Types of Cataract Removal
Routine Method: An l0-mm. opening is made in the eye. The cataract is removed, and the opening is closed with sutures.
Small Incision Cataract Surgery (SICS: An 5-mm. opening is made in the eye. The cataract is removed, and the opening needs so suturing as the opening is relatively small. This procedure similar to Phacoemulsification, but done manually without machinery support.
Phacoemulsification: Phacoemulsification is the most perfect and updated restorative operation for cataract. This could be further enhanced by using a foldable multifocal IOL. Advantages of Phaco surgery are
- Small Incision
- No sutures
- No hospital stay
- Negligible astigmatism
- Early recovery - resume normal life in 4-5 days
What are the risks of cataract surgery?
As with any surgery, cataract surgery poses risks, such as infection and bleeding. Before cataract surgery, your doctor may ask you to temporarily stop taking certain medications that increase the risk of bleeding during surgery. After surgery, you must keep your eye clean, wash your hands before touching your eye, and use the prescribed medications to help minimize the risk of infection. Serious infection can result in loss of vision.
Cataract surgery slightly increases your risk of retinal detachment. Other eye disorders, such as high myopia (nearsightedness), can further increase your risk of retinal detachment after cataract surgery. One sign of a retinal detachment is a sudden increase in flashes or floaters. Floaters are little "cobwebs" or specks that seem to float about in your field of vision. If you notice a sudden increase in floaters or flashes, see an eye care professional immediately. A retinal detachment is a medical emergency. If necessary, go to an emergency service or hospital.Your eye must be examined by an eye surgeon as soon as possible. A retinal detachment causes no pain. Early treatment for retinal detachment often can prevent permanent loss of vision. The longer the retina stays detached, the less likely you will regain good vision once you are treated.
Even if you are treated promptly, some vision may be lost. Talk to your eye care professional about these risks. Make sure cataract surgery is right for you.
What if I have other eye conditions and need cataract surgery?
Many people who need cataract surgery also have other eye conditions, such as age-related macular degeneration or glaucoma. If you have other eye conditions in addition to cataract, talk with your doctor. Learn about the risks, benefits, alternatives, and expected results of cataract surgery
What happens before surgery?
A week or two before surgery, your doctor will do some tests. These tests may include measuring the curve of the cornea and the size and shape of your eye. This information helps your doctor choose the right type of IOL.
What happens during surgery?
At the hospital or eye clinic, drops will be put into your eye to dilate the pupil. The area around your eye will be washed and cleansed.
The operation usually lasts less than one hour and is almost painless. Many people choose to stay awake during surgery.
Others may need to be put to sleep for a short time. If you are awake, you will have an anesthetic to numb the nerves in and around your eye.
After the operation, a patch may be placed over your eye.You will rest for a while.Your medical team will watch for any problems, such as bleeding. Most people who have cataract surgery can go home the same day.You will need someone to drive you home.
What happens after surgery?
Itching and mild discomfort are normal after cataract surgery. Some fluid discharge is also common.Your eye may be sensitive to light and touch. If you have discomfort, your doctor can suggest treatment. After one or two days, moderate discomfort should disappear.
For a few days after surgery, your doctor may ask you to use eyedrops to help healing and decrease the risk of infection. Ask your doctor about how to use your eyedrops, how often to use them, and what effects they can have.You will need to wear an eye shield or eyeglasses to help protect your eye. Avoid rubbing or pressing on your eye.
When you are home, try not to bend from the waist to pick up objects on the floor. Do not lift any heavy objects.You can walk, climb stairs, and do light household chores.
In most cases, healing will be complete within eight weeks.Your doctor will schedule exams to check on your progress.
For more information about cataract, you may wish to contact:
Counseling Department
Joseph Eye Hospital, Trichy-620001
Ph:0431-2460622